Health Operations Associate
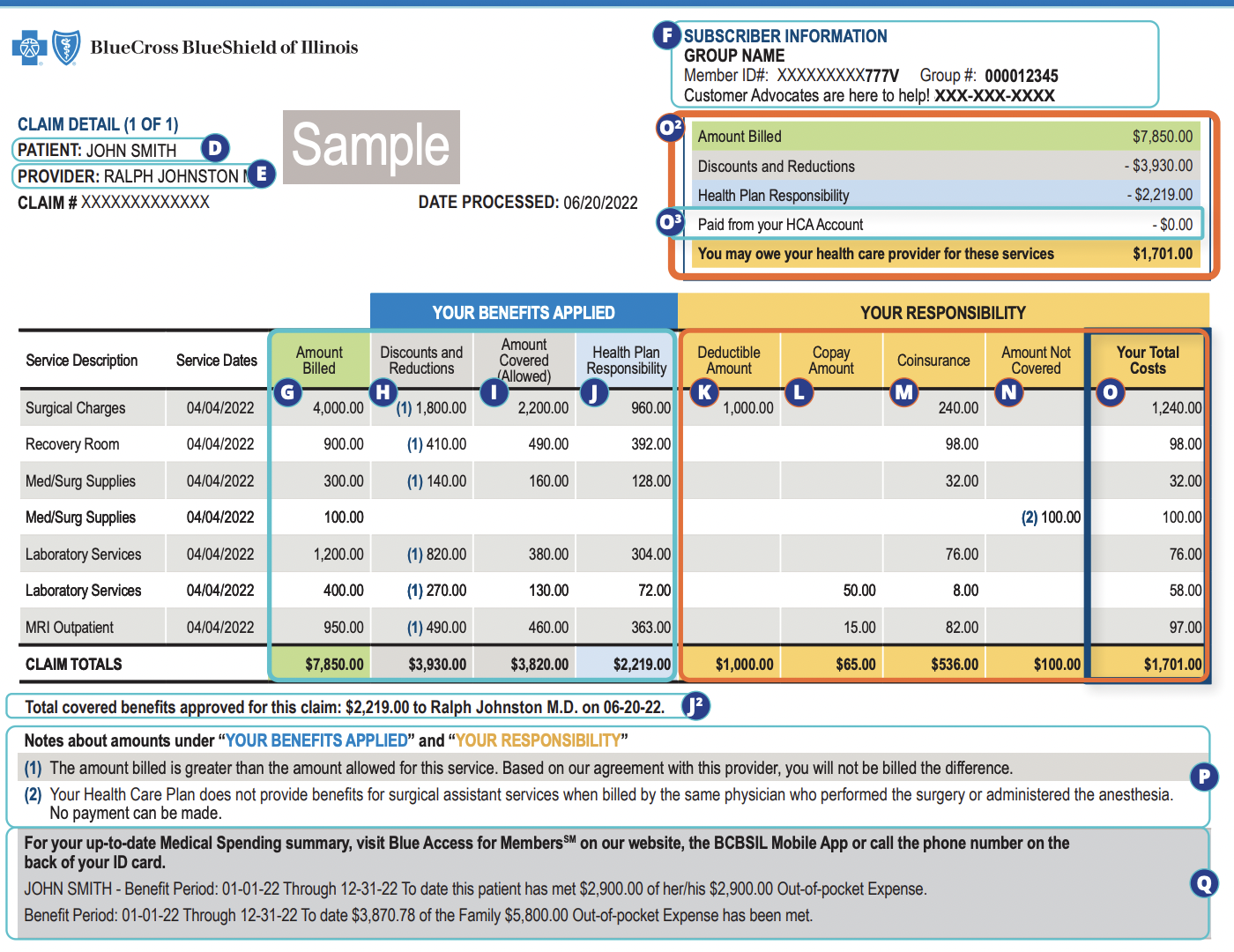
Experienced in processing provider and member-submitted claims, including verifying patient membership and eligibility, coordinating benefits, and managing pre-authorizations. Skilled in reviewing and updating medical records, applying accurate benefit coverage, pricing, CPT/ICD-10 codes, and revenue codes to ensure proper claim adjudication. Proficient in manual data entry, with strong attention to detail in validating NPI, tax ID, and provider information to support compliance and minimize claim denials.